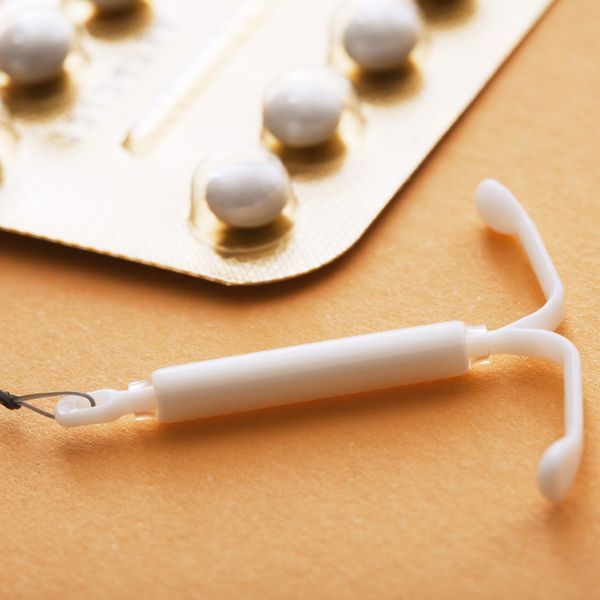
I remember the day of my wedding…when I started feeling my contraception ring coming out of my vagina. I had only recently started using the ring even though I was more used to taking the pill. There I was in the bathroom stall with one of my bridesmaids, and she was literally helping to guide my ring back up into my vagina because I could feel it slipping out of me. Although quite embarrassing, let's just say that we're forever bonded by that experience. So, have you ever tried a new birth control method that wasn't the best for you but it seemed to work well for others?
During a recent interview with Board Certified Obstetrician & Gynecologist, Dr. Chimsom Oleka, she provided a list of all of the birth control methods currently available, which can potentially serve as a starting point for those of you who may be exploring new contraceptive methods.* As you continue reading, you'll notice that the list is organized based on what Dr. Oleka refers to as Short-acting (hormonal and non-hormonal), to Long-acting, to Barriers of Protection.
Before we dive into the list, let's first clarify specifically what birth control does. As. Dr. Oleka explained, for most methods, birth control releases certain hormones in your body which contributes to the ultimate end goal: block ovulation or keep an egg from being released, thicken the mucus in the cervix so that sperm can't pass through, and/or thin the lining of the uterus, which decreases chances of implantation. Each birth control method is designed to do each or all of these things, but depending on the method, they will either do them better, worse, or not at all.
Choosing The Best Birth Control Method For You
SHORT-ACTING BIRTH CONTROL METHODS

Shutterstock
Note: Throughout this section, you will notice references related to "continuous" or "extended" usage. As Dr. Oleka explained, many of us have a false idea of what the period is supposed to do. Contrary to popular belief in terms of what our menstrual cycle does and why it's "necessary" every month, ultimately its main purpose is for pregnancy. That's it.
As Dr. Oleka expertly pointed out, "It's the birth control's period, not your period. Your birth control will start stimulating the lining and doing all of the things that cause you to bleed." So, as long as you have a hormone that's assisting with protecting and keeping your uterus lining thin, and as long as you've consulted your physician beforehand, then you don't have to necessarily worry about shedding the lining every month (i.e. having a period).
Consider, for example, women who have bleeding disorders (i.e. their bodies bleed too much or won't stop bleeding), female athletes, as well as those who may suffer with things such as menstrual migraines…situations like these support the case for continuous or extended methods.
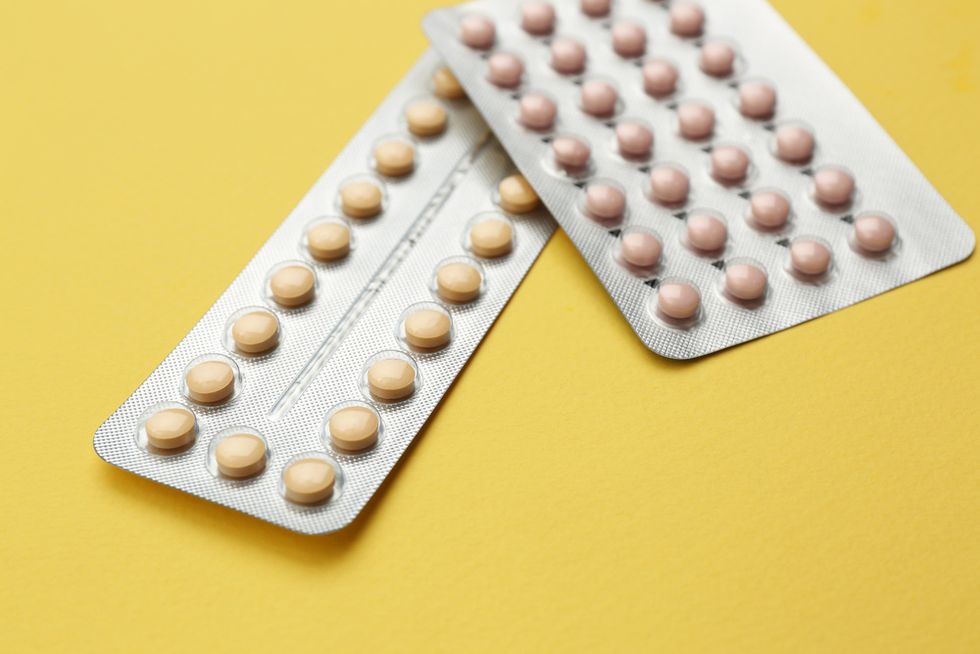
Method: Birth Control Pill (Hormonal - Estrogen and Progesterone)
Shutterstock
How It's Administered: Self-ingested orally, daily
Efficacy: 7 to 9% failure rate (i.e., approximately 1 in 10 will get pregnant)
Description & Overview:
Birth control pills usually come in 28-day pill packs (four rows of seven pills) including a week of placebo, non-active pills. There are different variations as well, but it's critical that you take it every day at the same time.
The most commonly used pill has both estrogen and progesterone. With estrogen, it tends to help provide more stability of the lining. However, some people may not want estrogen or they may have an underlying medical issue that conflicts with the estrogen. There is a risk of blood clots, although fairly low, but the risk of this goes up when you're pregnant. With the pill, it helps regulate the bleeding, which in turn, helps make it predictable. It's known to have protective benefits such as helping to decrease risk of certain cancers and it can help reduce symptoms related to fibroids.
Also, you can use this method, as well as other methods, continuously or in an extended way so that you can delay or skip the bleeding (i.e. going on vacation). For example, if you wanted to try an extended use, then you could delay the withdrawal bleeding (period) for a set number of weeks or months by skipping the last row for let's say two months. Then, you would take the last row of inactive pills the third month, so that you would only bleed approximately every 10 weeks.
On the other hand, if you're someone who decides "I don't want to bleed at all," then you could skip the last row of inactive pills and move forward with starting the new pack each month. Keep in mind, if you don't bleed or you bleed too heavily already, there may be other medical issues going on, so as always, you'll want to consult your physician about this.
Side effects can vary, but some of the most common side effects include: nausea, breast tenderness, and initial irregular bleeding.
Method: Birth Control Pill (Hormonal - Progesterone Only)
How It's Administered: Self-ingested orally, daily
Efficacy: 7 to 9% failure rate
Description & Overview:
This method basically works pretty much the same as the first pill mentioned above, but it doesn't include estrogen. It only includes progesterone.
Progesterone-only pills can be harder for some women to use because you have to be really consistent. If the daily pill ingestion time is missed by as little as three hours, then it loses its efficacy. Hence, it's critical that you take the pill every day at the same time.
With the progesterone-only pill, there's also a greater chance of irregular bleeding. Hence, this method is usually recommended by the physician if there are estrogen-related conflicting medical issues.
Method: Vaginal Ring (Hormonal – Estrogen and Progesterone)

Michael Kraus/Shutterstock
How It's Administered: Self-inserted through Vagina
Efficacy: 7 to 9% failure rate
Description & Overview:
The vaginal ring is a soft, flexible ring approximately two inches wide and four centimeters thick that is self-inserted and removed in/out of the vagina. Some women will tie a string to the ring and there's also an applicator that can be used to assist with insertion and removal.
The vaginal ring stays in for three weeks and releases hormones every day. Once removed for seven days, it allows withdrawal bleeding (period) to occur. Then, a new ring is inserted every four weeks. This method can be used continuously if you bypass the seven days and move forward with inserting the new ring every three or four weeks, or in an extended way if you bypass the seven days every few months or so.
The ring has been known to cause breakthrough or irregular bleeding. Not to mention, there are times when the ring can slip out during sex, which of course can directly impact the efficacy.
Method: Progesterone-Only Shot (Hormonal - commonly referred to as “Depo”, short for Depo Medroxyprogesterone Acetate)
How It's Administered: Injected in arm by physician
Efficacy: 6% failure rate
Description & Overview:
The progesterone-only shot is usually injected every three months (or every 11 to 13 weeks). Although the failure rate is approximately 6%, that's also related to the fact that patients are late with getting their scheduled shot.
Depo is known to decrease bone mineral density (contributes to the risk of fractures) within the first two years, but you start to recover it within 30 months after you stop taking it.
Also, because the shot can linger in your system up to nine months after your last shot (not the efficacy), it has the propensity to delay the return to your normal fertility state.
Some of the most common side effects include weight gain with research showing that it can act as an appetite stimulant.
Method: The Patch (Hormonal – Estrogen and Progesterone)

Michael Kraus/Shutterstock
How It's Administered: Self-adhesive
Efficacy: 7 to 9% failure rate
Description & Overview:
The patch is a small, square-shaped band-aid like adhesive or patch that can be applied to your upper arm, abdomen, or butt. You receive a new patch every three weeks and the fourth week is when you're patch free to allow for withdrawal bleeding.
This method is not recommended for extended or continuous cycles like with the pill and ring because it has higher levels of estrogen, which means increased risk for blood clots. Also, if you have sensitive skin or you're prone to breakouts and rashes, then you may want to avoid this method as well.
The patch can cause irregular or breakthrough bleeding or no bleeding at all depending on the individual. During the first few months of use, you may experience that as well as nausea, but it usually improves over time.
Method: Family Planning (Non-hormonal)
How It's Administered: N/A - Personal planning and scheduling
Efficacy: Up to 40% failure rate
Description & Overview:
There are a variety of options as it relates to family planning including: use of calendars, basal body temperature, cervical mucus, and more. There are a lot of useful tracking apps that can help with these methods as well.
Family planning can be taught and is a pretty well-accepted method. However, it can only be used if you have a regular cycle. Also, it has a very high failure rate because it requires extensive tracking and managing certain records such as time, ovulation, and temperature. So, you have to be extremely detailed-oriented, organized, and highly motivated to be successful with family planning. Otherwise, it can be extremely overwhelming for some people.
Due to the excessive planning and stringent scheduling, it can potentially decrease sexual spontaneity and/or convenience.
LONG-ACTING BIRTH CONTROL METHODS
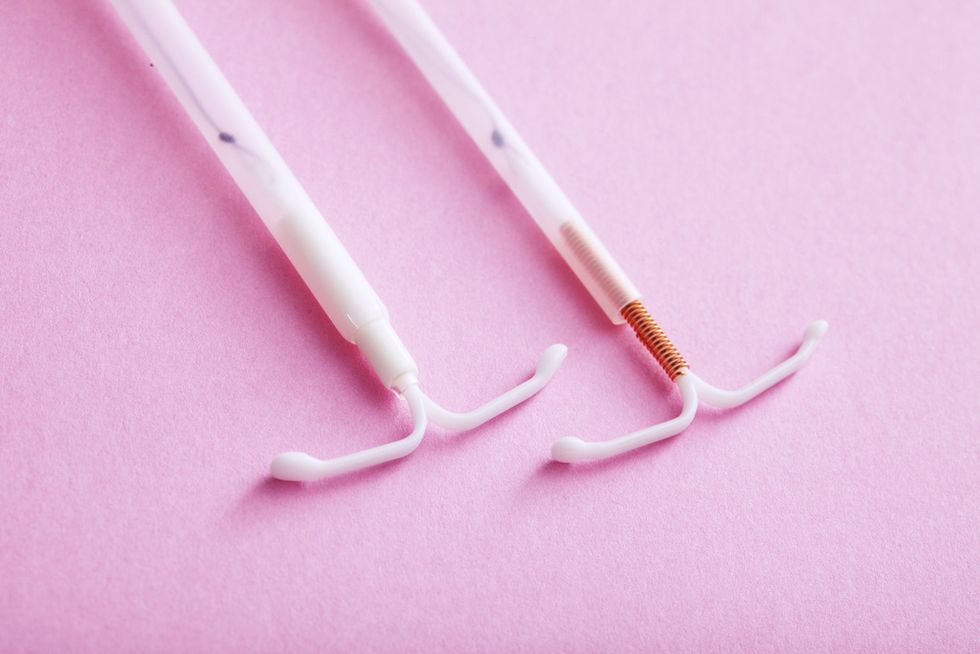
Method: IUD (Hormonal - Progesterone Only)
Shutterstock
How It's Administered: Inserted vaginally by physician (through opening of cervix, into the uterus)
Efficacy: Less than 1% failure rate
Description & Overview:
The IUD has varying brands (Mirena has been around the longest), costs, and dosages. The IUD is a small, t-shaped plastic piece, approximately 3 cm in size, although the size can vary as well. In addition to women who have had children, the IUD can be used in teenagers as well as women who have not have had babies.
Remember, this is a longer-acting method, so this is ideal for someone who wants to hold off on having children for a longer period of time.
Some of the most common side effects include insertional discomfort (I'm a personal witness to this) and irregular bleeding although it tends to help those who suffer from painful periods and heavy flow. The longer you leave it in, the less likely you'll bleed.
Method: Copper IUD (Non-hormonal)
How It's Administered: Inserted vaginally by physician (through opening of cervix, into the uterus)
Efficacy: Less than 1% failure rate
Description & Overview:
Similar to the IUD previously mentioned, the copper IUD is a latex-free, t-shaped, plastic piece but it also includes areas of exposed copper. By releasing copper salts into your body, the copper tricks the uterus into thinking something foreign is inside, creating an appearance of a "chaotic" environment in your system, which ultimately blocks sperm and prevents reproduction. It can last for 10 years, but it has been known to be effective for up to 12 years.
The copper IUD is ideal for someone who doesn't want to deal with hormones, or someone who is certain they don't want children for a long time. There are instances where it can be used as emergency contraception but it won't work if something has already been implanted.
Because this method doesn't affect ovulation, this method is also ideal for women who want to continue bleeding or women within certain cultures where the idea of contraception isn't readily accepted. This can serve as contraception method without anyone else truly knowing that you're taking it because you will still have a period as normal.
The most common side effects usually include more painful cramping or heavier bleeding.
Method: Contraceptive Implant (Hormonal – Progesterone Only)

Michael Kraus/Shutterstock
How It's Administered: Implanted in arm by physician
Efficacy: Less than 1% failure rate (the most effective method)
Description & Overview:
The contraceptive implant is a flexible, plastic rod that's placed inside the upper arm. It's small and thick - approximately 4 cm long and 2 mm thick. It releases hormones daily, and lasts for three years, although recent data shows it may last longer than that. After three years, you get a new one if you choose to do so. Otherwise, you will return back to your baseline fertility.
Some of the most common side effects can include irregular bleeding, no bleeding (approximately 6%), or heavier bleeding. For those who experience irregular bleeding, there are ways to decrease it and make it more manageable. Also, there are rare occasions where, if placed improperly, it can shift or migrate.
BARRIERS OF PROTECTION** BIRTH CONTROL METHODS
The most common effects for any of the following methods can include vaginal discharge and irritation. After the use of these, the return to fertility is usually fairly quick.
As it relates to a lot of these barriers of protection, Dr. Oleka likes to think of it this way, "Condoms should be used more so for STD and HIV/AIDS protection, and less for pregnancy prevention." Nevertheless, they are still considered methods for both pregnancy and STD/HIV prevention.
Method: Male Condom (Non-hormonal)

Michael Kraus/Shutterstock
How It's Administered: Applied by male on his penis
Efficacy: 15% failure rate (research across the board states this although it seems quite questionable by both the expert and the writer)
When to Apply: Right before sex
Description & Overview:
Condoms are usually latex or you can opt for lambskin if you're allergic to latex. However, anything non-latex has been known to be less effective in preventing pregnancy as well as STDs. With condoms, common things like inconsistent use, slippage during sex, and the risk of it tearing are a few factors that can directly impact the overall efficacy.
Method: Female Condom (Non-hormonal)
How It's Administered: Self-inserted vaginally
Efficacy: 21% failure rate
When to Apply: Right before sex
Description & Overview:
Similar to the male condom, the female condom has a thick ring that's used for placement within the vagina along with the pouch that goes in when it's time to have sex. There's also a thin ring that goes outside of the vagina. With this method, proper placement is just as important because it helps prevent condom slippage during sex. Also, the male condom should not be used when the female condom is used because it can cause tearing.
Method: Diaphragm

Shutterstock
How It's Administered: Self-inserted vaginally
Efficacy: 16% failure rate
When to Apply: Up to six hours before sex.
Description & Overview:
The Diaphragm is reusable silicon disk that's self-inserted through the vagina. Similar to the cervical cap, it should be inserted up to six hours before you have sex and should remain in your vagina at least six hours after sex. A spermicide should also be used in conjunction with the diaphragm to help ensure efficacy. It's also possible for the diaphragm to become dislodged during sex.
Method: Cervical Cap (Non-hormonal)
How It's Administered: Self-inserted vaginally
Efficacy: 14 to 20% failure rate
When to Apply: Up to six hours before sex
Description & Overview:
The cervical cap is a reusable silicone rubber cup that sits on the cervix while you're having sex. Think of it as a "hat" that comes in different sizes and sits on your cervix. It's usually inserted into the vagina up to six hours prior to sex, it should remain in there for at least six hours after sex (and can remain there up to 48 hours). Of note, it only works if used with a spermicide. There's usually only one brand available in the United States.
One thing to consider is proper placement of the cap, and making sure you're comfortable with putting it in your vagina. Also, if you've already had a baby, then you'll have a higher risk of contraception failure.
Additionally, here are a few things Dr. Oleka suggests women should consider before choosing a contraceptive:
- What are your chances of getting pregnant with this method (efficacy)?
- What do you want your bleeding profile to look like (i.e. how often do you want your "withdrawal bleeding" or menstrual cycle to occur)? How will this affect my bleeding profile?
- What does your lifestyle look like (i.e. will it be difficult to remember to take the pill every day versus another option that may not require as much involvement)?
- What are your priorities? What does the timeline for trying, starting, or growing your family look like?
- How long do you want it to be in effect or control?

Shutterstock
As always, Dr. Oleka reminds everyone to be sure and consult your physician* when deciding on a method because hormones affect individuals differently. Not to mention, there's certain criteria and health/risk factors that doctors review and consider when determining contraception needs for their patients.
With most methods, efficacy is usually effective within a week or so, but to be safe, Dr. Oleka suggests giving the new contraception at least a month or two to allow enough time to confirm efficacy on your side and to see how well your body reacts to it.
*Before taking any medications, over-the-counter drugs, supplements or herbs, consult a physician for a thorough evaluation. xoNecole does not endorse any medications, vitamins or herbs. A qualified physician should make a decision based on each person's medical history and current prescriptions. The prescribing physician should be consulted concerning any questions that you have.
**Quick note about Plan B: Plan B is NOT a standard contraceptive like those mentioned above. Conversely, it is an emergency contraceptive, and should be used as soon as possible after sex (within 72 hours, up to 5 days). Dr. Oleka recommends that you already have some beforehand to prevent from panicking or having to run around to find in the middle of the night trying to find an open local pharmacy.
Join our xoTribe, an exclusive community dedicated to YOU and your stories and all things xoNecole. Be a part of a growing community of women from all over the world who come together to uplift, inspire, and inform each other on all things related to the glow up. We drop xoNecole events and special opportunities into our Tribe first.
Featured image by Shutterstock
- The Difference Between Your Period And Ovulation - xoNecole: Women's Interest, Love, Wellness, Beauty ›
- Ari Lennox Shares Traumatic Story About Getting IUD - xoNecole ›
- Things You Might Not Know Affecting Your Fertility Issues - xoNecole ›
- Birth Control - Mayo Clinic Health System ›
- Which Birth Control Method Is for You? 19 Types, Pros, Cons, More ›
- Find Your Birth Control Method 2020 | Power to Decide ›
- Choose the Right Birth Control - MyHealthfinder | health.gov ›
- 5 types of birth control options: which is best for you ... ›
- Birth control options: Things to consider - Mayo Clinic ›
- Best Birth Control For Me Quiz | Choosing the Right Contraceptive ›
This Is How To Keep 'Holiday Season Stress' From Infecting Your Relationship
Hmph. Maybe it’s just me, but it seems like there is something really weird happening in the fall season air (because winter doesn’t officially begin until December 21) that cuddle season is in full swing while break-up season is as well. In fact, did you know that break-ups are so popular during the holiday season that December 11 is deemed Break-Up Day?
The reasons why relationships shift around this time vary; however, I did both roll my eyes and chuckle when I read that a very popular one is because it’s an easy way to get out of getting one’s significant other a Christmas present. SMDH.
Anyway, I personally think that the less shallow folks out here may contemplate calling things “quits” or they at least distance themselves a bit from their partner (and what I’m referring to is serious relationships) due to all of the stress and strain that oftentimes comes with the holidays whether it be financial, familial, due to their tight schedules or something else.
Listen, I would hate for you and your man to miss the fun and happiness of experiencing this time of year, all because you are so overwhelmed or irritated that you can’t really enjoy it. That’s why I have a few practical tips for how to avoid allowing the typical holiday season stress from INFECTING your relationship.
Manage Your Expectations
 Giphy
GiphyUnmanaged expectations. If there is a main reason why the holiday season tends to be so stress-filled for so many people, I’d bet good money that this is the cause. And when you’re in a long-term relationship, expectations can manifest themselves in all sorts of cryptic and/or unexpected ways. You might have relatives who assume that you are going to be with them for Thanksgiving or Christmas when you have other plans in mind. You might be thinking that you are going to spend one amount for presents while your man is thinking something totally different. When it comes to scheduling, your signals may be crossed.
And you know what? To all of these scenarios, this is where clear and consistent communication come in. Don’t assume anything. Don’t dictate anything either. From now until New Year’s, mutually decide to check in once a week, just to make sure that you are both on the same page as it relates to the holidays and what you both are thinking will come along with it. The less blindsided you both feel, the less stressed out you will be. Trust me on this.
Set (and Keep) a Budget
 Giphy
GiphyOkay, so I read that last year, 36 percent of Americans incurred some type of holiday-related debt. Hmph. Last year, there was still some sense of normalcy in this country, chile, so I can only imagine what finances are gonna look like over the next several weeks. That said, since I don’t know a lot of people who don’t find being broke stressful, make sure that you and your bae set a budget and then stick to it this year — no ifs, ands or buts.
Because really, y’all — it doesn’t make sense to deplete savings and/or max out credit cards for a few days of giggles only to be damn near losing your mind because you don’t know how to make ends meet come Dr. Martin Luther King, Jr. Day.
And by the way, this tip doesn’t just speak to things like food and gifts; I also mean travel. If it doesn’t make a ton of sense (or cents) to be all over the place this year — DON’T BE.
Keep Matthew 5:37 at the Forefront
 Giphy
GiphyIf off the top of your head, you don’t know what Matthew 5:37 says, no worries, here ya go: “But let your ‘Yes’ be ‘Yes,’ and your ‘No,’ ‘No.’ For whatever is more than these is from the evil one.” That verse right there? Oh, it’s a boundaries lifesaver! I say that because do you see “maybe” or “I’ll think about it” in there? Nope. LOL. It says that you should tell people “yes” or “no” and leave it at that — and that complements Anne Lamott’s quote, “’No’ is a complete sentence” impeccably well. Yeah, you’ve got to remember that anything beyond a yes or no to a request is privileged information; you don’t owe anyone details or an explanation.
Besides, if you are really honest with yourself, when someone asks you something and you give a “Umm, let me think about it” kind of reply, more times than not, you already know what your answer is going to be — so why not let you both off of the hook? Give your response. Commit to that. And let everyone (including yourself) get on with their lives and schedules.
I promise you that when it comes to those holiday parties, you are pissing more folks off by not RSVP’ing or doing so and not showing up than just saying, “Thank you but not this year” off the rip.
Remember That Your Personal Space Is Privilege Not a Right
 Giphy
GiphyA friend of mine recently bought a new house and invited me over to come see it. He’s a single man with no children, so as I was taking in all of the space that he had, especially as I walked through his finished basement, I joked about relatives coming to live with him. “Hell no” and “absolutely not” were pretty much his immediate responses as he went on to say that some folks even had the nerve to be offended when he told them that he had no intentions on taking DNA in.
Ain’t it wild how people think that your stuff is their right? And yes, that brings me to my next point. Your home is your sanctuary space. If you want to host folks this year — cool. If not, ALSO COOL. Please don’t let folks (family included) guilt you into how they want you to act or even into what they would do if the shoe was on the other foot. You are not them — and as one of my favorite quotes states, “If two people were exactly alike, one of them would be unnecessary.” (A man by the name Larry Dixon said that.)
Hell, my friends? They know that I am good for sending them random things that they need or even want all throughout the year. Coming over to hang out at my pace, though. Uh-uh. Chalk it up to being a card-carrying member of the ambivert club yet I like keeping my living space personal — and I sleep like a baby, each and every night, for feeling that way.
Always remember that your space, your time, your resources, your energy and shoot, yourself period (including your relationship), are all things that are your own. You get to choose how, when and why you want to share them. The holiday season is certainly no exception.
Cultivate Some “You Two Only” Traditions
 Giphy
GiphyIt’s not uncommon for some couples to hit me up after the holiday season to “detox.” Sometimes it’s due to the financial drama (and sometimes trauma) that they experienced. Sometimes it’s because they allowed their relatives (especially in-laws) to get more into their personal business than they should’ve. More than anything, though, it tends to be because they didn’t get enough quality time together and so ended up feeling “disconnected.”
Please don’t let that happen. Listen, I’m not even a holidays kind of woman and yet, I will absolutely sit myself down with some hot chocolate and chocolate chip cookies to enjoy a Hallmark holiday film or two. Aside from the fact that most of them are lighthearted and sweet, I also like that they usually focus on couples loving on each other amidst all of the holiday beauty and ambiance — which is something that all couples should set aside some time to do.
Maybe it’s a vacation. Maybe it’s a staycation. Or maybe it’s my personal favorite, A SEXCATION. Whether it’s for a few days, the weekend or even overnight — don’t you let the holidays go by without setting aside time for you and your man to celebrate one another. Don’t you dare (check out “Are You Ready To Have Some Very Merry 'Christmas Sex'?”).
GET. SOME. REST.
 Giphy
GiphyI once read that 8 out of 10 people get stressed out over the holidays and 3 out of 10 lose sleep during to it — and when you’re stress-filled and sleep-deprived, that can absolutely lead to hypersensitivity, making mountains out of molehills and even not being in the mood for sex.
Your relationship can’t afford to go through any of this, so definitely make sure to prioritize rest. I don’t care how unrealistic it might seem during this time, sleep should never be seen as a luxury; it will always and forever be a great necessity.
That said, try to get no less than six hours of shut-eye in (check out “6 Fascinating Ways Sex And Sleep Definitely Go Hand In Hand”) and even ask your bae to take a nap with you sometimes (check out “Wanna Have Some Next-Level Sex? Take A Nap, Sis.”). Not only will sleep help to restore your mind, body and spirit but, when it’s with your partner, it’s an act of intimacy that can make you both feel super connected, even in the midst of what might feel like chaos.
___
Holiday season stress is real. Still, never give it the permission or power to throw your relationship off. Put you and your man first and let the holidays be what they are gonna be, chile.
Let’s make things inbox official! Sign up for the xoNecole newsletter for love, wellness, career, and exclusive content delivered straight to your inbox.
Featured image by Shutterstock
'Constant Reassurance' Is The Relational Orange Flag No One Wants To Address
Read more than scroll. Boy, if there is a motto that I would encourage people to implement, now more than ever in their life, it would be how important it is to read (actual books, researched data and fact-based information) over merely scrolling via social media. Because boy — every time I look out on apps to see what folks are talking about, I don’t know if I’m impressed with or appalled by how many nothing-more-than-emotionalized opinions are so boldly stated when, after five minutes on Google, it’s clear that there are virtually zero facts to back them up.
Not to mention the fact that so many folks literally don’t read (you know, past skimming) anymore — and yes, I have stats to prove it. I recently read that back in 2022, reportedly, a little over 48 percent of people read one book over the course of that entire year (that is not a good thing and proves that book reading is on a steady decline). Meanwhile, the amount of time that is spent on social media: 2.5 hours on a daily basis. That’s 150 minutes of listening to folks just say…whatever. And if you listen to it long enough, you could actually start believing it as gospel.
This includes what I am going to touch on today: the belief that if someone really cares about you, they should constantly reassure you. Y’all damn near are gonna have me join the world of social media again, just to address this one fallacy. For now, though, I’ll settle for making some points via this article — because as you can see from the title, I don’t agree with that conclusion at all.
In fact, I personally believe that thinking this way is a pretty big relational orange — if not red — flag.
Reassurance. And What It Does for a Child.
 Giphy
GiphyIf you’ve read enough of my content, you know that I am big on word definitions — and when it comes to the word “reassurance,” the meaning alone explains why this article has the title that it does:
Reassurance: something, such as information, praise, or an action or gesture, that soothes, comforts, or restores to confidence
Reassurance restores confidence. Bookmark that, please. I will certainly circle back to that point before I am done.
Okay, so when it comes to, say a child, there is absolutely a place for reassurance. That’s because they are still in the process of significant self-development and so they need reassurance in order to feel safe, secure and loved. It’s also a way for them to establish trust in others.
However, did you know that many mental health experts say that if a child deals with, say anxiety, constant reassurance can actually be counterproductive because they can start to rely on external validation to emotionally stabilize them instead of learning how to remain calm and relaxed on their own (yeah, bookmark that too)? Some other ways that constant reassurance can become potentially problematic is it can cause kids to create problems that don’t exist, to overthink and to jump to the wrong conclusions (hmm…very interesting).
And so, already, we’re seeing something pretty interesting, right? Although reassurance has its place, too much of it, even for kids, typically ends up doing more harm than good.
Let’s keep building.
How 'Lack' As a Child Can Manifest As an Adult
 Giphy
GiphyOkay, so we just touched on how constant reassurance can be counterproductive for an anxious child. Now what about when that child grows up? If they never learned how to properly and effectively deal with their anxiety, what then? Well, this is where attachment styles can very easily come into play — especially since one of them is literally called “anxious attachment style.”
Anxious attachment style is rooted in insecurity. It typically stems from experiencing the type of dysfunctional upbringing that resulted in one or both parents being unpredictable or inconsistent in their caregiving approach and techniques. As a result, the child deals with things like fear of abandonment or rejection and, without healing from that, they become an adult who is pretty much the exact same way.
In relationships, it can manifest in them being extra clingy, codependent, super jealous, controlling or — catch it — someone who is always looking for validation and reassurance.
Hmph. Did you catch that? Did you really catch that? Needing constant reassurance in a relationship IS NOT something that should automatically come with a relationship. In fact, if you’re someone who has this type of need or even expectation, there’s a really good chance that what you actually need is therapy — not for your partner to work harder to make you feel better about yourself or the relationship.
Which brings me to my next point.
Relationships Can Be Therapeutic. They Aren’t Therapy, Though.
 Giphy
GiphySomething that some of my clients will tell you that they’ve heard me say, more than once I might add is, “PARENT and PARTNER are not palindromes.” A palindrome is a word (line, sentence, etc.) that is the same whether it is spelled backwards or forwards — and while, of course, parent and partner couldn’t qualify as being that, what I mean is there are far too many people who think that partners should pick up where parents left off and/or dropped the ball — and that is a super unhealthy approach to relationships. Come to think of it, not only is it unhealthy but really unfair as well.
This is exactly why I’m not big on phrases like “the princess treatment” in adult relationships. A princess is the daughter of a king while a queen is the wife of one. For a grown woman to expect a man to do what a father did for her as a child without accepting that as an adult, there are far more responsibilities as a wife that comes into play? Yep, that is toxic thinking.
And you know what? So is expecting your partner to overcompensate for where your father and/or mother didn’t show up in the way that they should have. That is not your partner’s fault, their role or their assignment while dating you. If you feel otherwise, it really is time to speak with a professional who can help you to do a bit of “reprogramming” in your thinking because, for you to feel and/or assume that since your parents didn’t make you feel confident and secure or teach you how to value yourself, your partner should work overtime to make up for it? There is not one thing that is healthy, mature or emotionally solid about having that type of mindset.
And that is why I am also good for saying that, although relationships can be therapeutic (healing), they should never EVER be seen as therapy. Therapists are trained to deal with the mental and emotional challenges that people have. On the other hand, no one should expect their partner to have the knowledge and expertise that professionals do — and while we’re here, partners also shouldn’t trust that someone who needs the assistance of a therapist to become whole (again) would know exactly what steps are required for that to happen.
So yeah, if you’re someone who thinks that being loved means that someone needs to constantly make you feel good about yourself or secure in the relationship — you probably do have an anxious attachment style. See a professional to get that confirmed, though. Because no one should have to make you feel valued or worthy. That is an inside job.
And this brings me to my final point.
It’s Not Fair to Want Someone to Love You More than You Do
 Giphy
GiphyFor this last point, something that Christ once said immediately comes to mind:
“No one puts a piece of unshrunk cloth on an old garment; for the patch pulls away from the garment, and the tear is made worse. Nor do they put new wine into old wineskins, or else the wineskins break, the wine is spilled, and the wineskins are ruined. But they put new wine into new wineskins, and both are preserved.” (Matthew 9:16-18 — NKJV)
A lot of times, Christ spoke in parables because it was easier for people to get where he was coming from (Matthew 13:13). Anyway, along these lines, what would be the point in pouring a liquid into a bottle that has a hole in it? It’s not built to contain and maintain the fluid and so, no matter how delicious the drink may be, no matter how many times it’s poured into the bottle, the bottle is never going to remain full — because it has cracks in it.
BOOKMARK THAT.
My fourth baby’s daddy (check out “Why I Named The Children I Aborted”), while we were in the process of our “exit interview” (which is what I choose to call it) of our dynamic, he said something that has always stayed with me: “Shellie, your biggest problem is you receive compliments are revelations when they should be seen as confirmations.” Hmph. The irony of HIM saying that is kind of a trip and yet, at the time when we were experiencing each other, he was exactly right. I should’ve never had such a low sense of self-worth that whatever a man said to me had me so in awe that I either felt extremely grateful or became super addicted to his validation.
And y’all, that is exactly what needing constant reassurance looks like — because why does someone need to keep telling you that you are beautiful, keep saying that you are wonderful, keep letting you know that they want to be with you — keep restoring your confidence in yourself and in your relationship with them?
In other words, why should they work harder at making you feel good about yourself and solid in your relationship than you are willing to? Isn’t that just like pouring liquid into a broken bottle?
There is someone in my family tree who I had to distance myself from because he kept venting to me about his marriage and the fact that his wife was just like this. Sadly, it was never (and I do mean NEVER) enough that he chose her — whenever she felt some type of way about herself, here she came looking for him to fill her voids. After a couple of years of the nonstop needs for reassurance, he was worn out from doing it and I was exhausted from hearing about it. He was too scared to call her out and she was too unaccountable to get the real help that she needed. Whew. Toxic on top of toxic.
So Shellie, what are you saying — that we shouldn’t expect compliments, affirmations, support and encouragement in our relationships? Chile, if that is what you got out of this, you are choosing to think that way because that couldn’t be further from where I am coming from.
Again, you’ve got to remember what reassurance means: it’s about restoring confidence. A compliment is “an expression of praise, commendation, or admiration” yet if you already know that you are pretty, smart, funny, whatever, someone telling you that isn’t “building your confidence;” it’s cosigning on something that you are already aware of. Encouragement is about inspiring or stimulating someone and so yes, of course, the right partner is going to want to see you win in life and so they are going to offer up influence and motivation to help you — but what if they aren’t there?
Shouldn’t you be able to encourage yourself? ABSOLUTELY. However, expecting them to restore your confidence due to things that have nothing to do with them or because you simply lack self-confidence? That is not how relationships are to go. If you aren’t sure of yourself (which is a foundational definition of confident), get to the root of why and then figure what you need to do to become sure — that way, your partner doesn’t have to constantly “fill you up;” actually, what they do will be surplus instead of void-filling because your “bottle” will be unbroken.
____
I’m telling you, if you pay attention to the relationship side of socials, at least twice a day, someone will talk about how they think that a relationship should entail receiving constant reassurance. Lies on top of lies. No one should think that love means trying to make someone else feel sure about themselves because they don’t know how to do so on their own.
And this is why I say that expecting constant reassurance is an orange, if not red, flag.
Because when you already feel good about yourself, there is no need.
And if you don’t, figuring out how to is an inside job — FIRST.
Let’s make things inbox official! Sign up for the xoNecole newsletter for love, wellness, career, and exclusive content delivered straight to your inbox.
Featured image by Shutterstock









